Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124
Physical Address
304 North Cardinal St.
Dorchester Center, MA 02124

Reviewed by: Dr. Urooj Fatima, Clinical Health Reviewer Last Updated: March 31, 2026 Disclaimer: This article is for educational and career guidance purposes only. Program costs, certification requirements, and scope of practice vary by state and institution. Verify current accreditation status and licensing requirements directly with CAAHEP, ABHES, or your state medical board before enrolling.
The medical assistant role is one of the most misunderstood positions in American healthcare. It is not a stepping stone to nursing, and it is not a glorified receptionist job. It is a genuinely dual-function clinical role — one that requires you to take a patient’s blood pressure and document their chief complaint in the exam room, then walk to the front desk and resolve an insurance pre-authorization issue before the physician finishes reviewing the chart.
Medical assistant programs exist to build that specific combination of skills in a compressed timeframe. Done well, the training produces someone who can function effectively in both the administrative and clinical dimensions of a medical practice on day one.
This guide explains how accredited programs actually work, what the training covers at each stage, what distinguishes good programs from poor ones, what the certification pathways look like, and what the work environment genuinely demands — including the parts most school websites leave out.
Who This Guide Is Relevant For:

Most job descriptions list bullet points. Here is what the dual role looks like in an actual 8-hour shift at a family practice clinic.
The morning starts with rooming patients — bringing them from the waiting room, recording current medications, taking vitals (blood pressure, heart rate, temperature, oxygen saturation, weight), and entering the chief complaint into the EHR before the physician enters. For a busy practice, this happens 15 to 25 times per day.
Between patients, the same assistant may be processing prior authorization requests for a prescription the physician wrote two days ago, calling a patient to relay lab results, or restocking the exam room supply cart. Depending on the practice’s size and staffing model, there may also be phlebotomy involved — drawing blood for in-house lab panels.
On the administrative side: scheduling follow-up appointments, scanning and filing documents into the EHR, verifying insurance eligibility before visits, and managing referral paperwork.
The pace is fast, the task-switching is constant, and the margin for error — particularly around medication documentation, vital sign recording, and patient identification — is narrow. That reality is what accredited training programs are designed to address before you enter a clinical setting.
The foundational phase covers the knowledge base required before any hands-on work begins. Core subject areas include:
This phase runs approximately 3 to 5 months in certificate programs. The quality of instruction here varies significantly between schools — a point covered in the program selection section below.
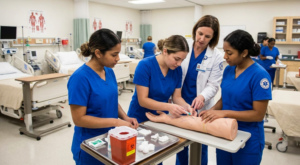
After the didactic component, students move into supervised lab practice. This is where procedural skills are built on mannequins and simulation equipment before any patient contact occurs.
Skills covered in this phase include:
The lab phase is where students discover whether they are actually comfortable with clinical procedures. An externship is not the time to realize that injections cause significant anxiety — the supervised lab environment is.
The externship is the final and most operationally significant phase of any accredited medical assistant program. Students complete a minimum of 160 hours (CAAHEP standard) of supervised practice in an actual clinical setting — typically a physician’s office, clinic, or outpatient facility.
This phase is unpaid in most programs, which is a financial consideration worth planning for. The externship site is usually arranged by the school, but students may sometimes request specific placement preferences.
What happens during the externship largely determines employment outcomes. Students who engage actively — asking questions, demonstrating initiative, showing up consistently — frequently receive job offers from their externship site before graduation. The externship is, in practice, a 160-hour working interview.
This point deserves more emphasis than most guides give it.
There are two accrediting bodies recognized for medical assistant programs in the United States:
CAAHEP — Commission on Accreditation of Allied Health Education Programs ABHES — Accrediting Bureau of Health Education Schools
Graduating from a CAAHEP- or ABHES-accredited program is a prerequisite for sitting the Certified Medical Assistant (CMA) examination administered by the AAMA, and the Registered Medical Assistant (RMA) examination administered by AMT.
A program that is not accredited by either body may be legally permitted to operate and may even grant a diploma. But its graduates cannot sit for the national certification examinations that most employers require. This is not a minor distinction — it is the difference between a credential that opens doors nationally and a certificate that may not be recognized outside the building where it was issued.
Before paying any tuition deposit, verify the program’s accreditation status directly on the CAAHEP or ABHES website. Do not rely on the school’s marketing materials.
| Factor | Certificate / Diploma Program | Associate of Science Degree |
|---|---|---|
| Duration | 9–12 months | 18–24 months |
| Typical Cost | $5,000–$15,000 | $8,000–$25,000 |
| General Education | Minimal or none | Required (English, Math, Sciences) |
| Career Focus | Immediate workforce entry | Longer-term advancement platform |
| Offered At | Vocational/trade schools | Community colleges |
| CMA/RMA Eligibility | Yes (if CAAHEP/ABHES accredited) | Yes (if CAAHEP/ABHES accredited) |
| Advancement to MLS or Nursing | Difficult without additional credits | Easier — credits may transfer |
The certificate pathway is appropriate for candidates who need to enter the workforce quickly and have a clear employment target. The associate degree is the better investment for anyone who may want to advance into a supervisory role, pursue further healthcare education, or wants the academic foundation that a general education curriculum provides.
One underappreciated consideration: community college associate programs are typically significantly cheaper per credit hour than private vocational schools offering certificates. The certificate may be faster, but it is not always less expensive in absolute terms.
CMA (AAMA) — Certified Medical Assistant Administered by the American Association of Medical Assistants. Requires graduation from a CAAHEP- or ABHES-accredited program. The examination covers clinical procedures, administrative functions, and general medical knowledge. Certification must be renewed every 60 months through continuing education or re-examination.
RMA (AMT) — Registered Medical Assistant Administered by American Medical Technologists. Accessible through accredited program graduation, military training equivalency, or documented work experience. Slightly broader eligibility criteria than the CMA.
CCMA (NHA) — Certified Clinical Medical Assistant Administered by the National Healthcareer Association. Does not require graduation from an accredited program — it requires passage of the examination and can be obtained through documented work experience alone. This makes it accessible but also means it carries less weight with employers who specifically require CMA or RMA credentials.
Which certification matters most to employers?
In most physician practice settings, CMA(AAMA) is the gold standard. Hospital systems and larger healthcare networks increasingly specify CMA or RMA in job postings. CCMA is recognized but is more commonly seen in urgent care and retail health settings.
Several patterns emerge consistently when physicians and practice managers evaluate newly graduated medical assistants — and most of them are never addressed in program curricula.
The EHR Confidence Gap
Students learn EHR concepts in classroom settings but typically have hands-on experience with only one system (often a training version of Practice Fusion or NextGen). Real-world practices use a range of platforms — Epic, Athenahealth, eClinicalWorks, Kareo — and each has a meaningfully different workflow. New graduates who understand the underlying logic of EHR systems (why fields exist, how billing links to clinical documentation) adapt quickly. Those who memorized click sequences in a training environment struggle.
Vital Signs Are Not As Simple As They Look
Manual blood pressure auscultation — using a stethoscope and sphygmomanometer rather than an automated cuff — is a skill that degrades quickly without practice and is performed poorly by a significant proportion of newly trained assistants. An incorrectly recorded blood pressure reading can result in unnecessary medication escalation or, conversely, a missed hypertensive urgency. Supervisors notice this gap immediately.
Patient Communication Is Undertrained
Most programs emphasize procedural skills. Few adequately prepare students for the communication challenges of actual patient interaction — managing an anxious patient before a blood draw, communicating a physician’s instructions to a patient who does not understand them, or handling a patient who is upset about a billing error. These situations arise daily and are not resolved by procedural competence alone.
The Scope of Practice Problem
Medical assistants in some states operate under broader scope than others. Students trained in one state who relocate may inadvertently perform tasks that exceed their authorized scope — or may be underutilized because their new employer has more restrictive policies. Understanding your state’s specific MA scope of practice regulations is not optional professional knowledge.
Prioritizing location over accreditation status
A school 5 minutes from your home that is not CAAHEP or ABHES accredited produces a credential of limited utility. An accredited program 30 minutes away produces a credential that qualifies you for national certification and is recognized by employers across all 50 states.
Not asking about externship placement specifics
The question is not “do you offer an externship?” — all accredited programs do. The question is “where are your students currently placed, and what percentage receive job offers from their externship site?” A school with strong hospital system and multi-specialty clinic partnerships produces meaningfully better employment outcomes than one placing students exclusively in small solo practices.
Skipping certification after graduation
Some graduates move directly into employment without sitting for the CMA or RMA examination, particularly if an employer hires them without requiring it. This is a short-term decision with long-term costs. Certification is portable — it follows you across employers and states. Non-certified experience is not recognized in the same way when you change jobs or relocate.
Assuming all hybrid programs are equivalent
Online theory components vary enormously in quality. The laboratory and externship hours cannot be completed online regardless of what a program advertises. If a school is claiming you can complete “everything online,” that program is not meeting CAAHEP or ABHES accreditation standards and likely is not accredited.
Family Practice and Internal Medicine
The broadest and most common placement. Patient volume is high, age range is wide, and the clinical variety — from pediatric well-checks to chronic disease management in elderly patients — requires adaptability. Expect a fast pace with less specialization.
Specialty Clinics
Cardiology, dermatology, orthopedics, gastroenterology, and similar settings involve a narrower patient population but deeper procedural involvement. A cardiology MA will become proficient in ECG interpretation artifacts and cardiac monitoring equipment. A dermatology MA will assist with skin biopsies, cryotherapy, and lesion documentation. Specialty roles frequently pay higher than general practice.
Urgent Care Centers
Higher acuity than a physician’s office, faster turnover, and a rotating physician model. The pace is demanding and the case mix unpredictable. These settings are excellent for developing clinical confidence quickly but require solid procedural foundations before starting.
Federally Qualified Health Centers (FQHCs)
Community health centers serving underserved populations. Often more clinically complex due to patient socioeconomic factors and delayed-presentation disease. FQHCs frequently offer loan repayment programs and government employee benefits. For candidates motivated by community health equity, this is a meaningful setting.
Telehealth Support Roles
An expanding area post-2020. Medical assistants in telehealth support roles manage patient intake, coordinate pre-visit diagnostic testing, and handle post-visit follow-up. This is less hands-on clinically but requires strong EHR and communication skills.
| Setting | Entry-Level (0–2 years) | Mid-Career (3–7 years) | CMA Premium |
|---|---|---|---|
| Family Practice (national median) | $36,000–$42,000 | $44,000–$52,000 | +$2,000–$5,000/yr |
| Specialty Clinic | $40,000–$47,000 | $50,000–$60,000 | Varies |
| Urgent Care | $38,000–$45,000 | $46,000–$54,000 | +$3,000/yr average |
| FQHC / Community Health | $38,000–$46,000 | $48,000–$56,000 | + loan repayment |
| Hospital Outpatient | $42,000–$50,000 | $52,000–$62,000 | Higher union benefit structures |
Geographic variation is significant. California, Washington, Massachusetts, and New York consistently show higher MA wages than national medians. Rural placements may include loan repayment or housing benefits that offset lower base salaries.
[IMAGE: Side-by-side comparison of a CAAHEP accreditation seal and an ABHES accreditation seal displayed on a school program page | ALT TEXT: “CAAHEP and ABHES medical assistant program accreditation seals used to verify legitimate CMA certification eligibility” | Use official accreditation seal images or a clean graphic showing both logos side by side. This is a high-value trust signal image — readers evaluating programs will find it immediately useful, and it reinforces the E-E-A-T accreditation emphasis that distinguishes this article from generic school-marketing content.]
Before enrolling:
During the program:
After graduation:
Withdraw your enrollment inquiry immediately if:
How long do medical assistant programs take?
Accredited certificate programs typically run 9 to 12 months. Associate degree programs run 18 to 24 months. Both pathways qualify graduates to sit for national certification examinations, provided the program holds CAAHEP or ABHES accreditation.
Can I complete a medical assistant program online?
The didactic component of many accredited programs is available in hybrid or online format. The clinical laboratory hours and the externship cannot be completed remotely — they require physical presence in a clinical setting. Any program claiming a fully online completion pathway is not meeting accreditation standards.
What is the difference between a medical assistant and a licensed practical nurse (LPN)?
LPNs complete a 12 to 18-month licensed nursing program and operate under nursing scope of practice, which includes medication administration, wound assessment, and IV care in most states. Medical assistants operate under physician supervision with a scope of practice defined by state law, which is narrower and specifically excludes independent nursing judgment. LPN programs are more academically intensive and more expensive; medical assistant programs are faster and more accessible.
Is certification legally required in every state?
No state currently mandates certification by law for the medical assistant title. However, most employers — particularly physician practices and hospital systems — require CMA, RMA, or equivalent credentials as a hiring condition. In practical terms, entering the job market without certification significantly limits your options.
Is this career suitable for a second-career adult over 40?
The physical demands — extended time on your feet, frequent movement between rooms, occasional lifting — are relevant considerations for anyone entering the field, regardless of age. The communication and organizational skills that come with life experience are genuinely valued in clinical settings. Many successful medical assistants enter the field as second careers. The question is less about age than about realistic physical stamina assessment and financial planning for the training period.
What does the CMA examination cover?
The CMA(AAMA) examination is divided into three content domains: General (medical terminology, anatomy, psychology, professionalism), Administrative (health information management, patient scheduling, insurance processing), and Clinical (infection control, patient preparation, clinical procedures, medication administration). The exam consists of 200 questions with a 3-hour time limit.
Can I work in a hospital as a medical assistant?
Yes, though hospital-based roles are less common than outpatient clinic placements. Hospital outpatient departments, specialty clinics affiliated with hospital systems, and procedural suites frequently employ certified medical assistants. Hospital positions typically offer stronger benefits packages and higher base wages than independent practices.
This article was reviewed by Dr. Urooj Fatima and is intended for educational and career planning purposes only. Accreditation status, certification requirements, scope of practice regulations, and salary data are subject to change. Always verify current information directly with CAAHEP, ABHES, AAMA, and your state medical board.